Leukemia study restores silenced gene in mice. Could it point to new treatments for humans?
Article | April 2, 2026

(Farmington, Conn. – April 2, 2026) – A key cancer-fighting gene in leukemia is switched off—not broken—and scientists from The Jackson Laboratory (JAX) found a way to switch it back on.
In a study published in Science Translational Medicine, the team revealed not only a potential new way to treat acute myeloid leukemia (AML) without harsh chemotherapy, but also a promising strategy to study more gene-silencing mechanisms in other diseases.
“If we can identify which genes have been silenced and understand how to turn them back on, that could open up entirely new therapeutic possibilities,” said Eric Wang, a JAX assistant professor who led the research. “Instead of only trying to kill these cells, we may be able to restore the mechanisms that normally keep them under control.”
An epigenetic switch
In normal cells, tumor-suppressor genes keep cells from becoming cancerous. But in leukemia and other diseases, some of these genes are switched off not because of DNA mutations that break them, but because cancer cells “silence” them while leaving them intact. Called “epigenetic” mechanisms, these changes to gene activity are notoriously difficult to track because standard DNA sequencing technologies rely on finding mutations or changes to DNA’s letters.
“Clinicians design treatments based on DNA sequencing that detects mutations,” Wang said. “But they don’t have any other method to detect epigenetic mechanisms that are also associated with really poor outcomes and cannot be sequenced.”
To counter that challenge, Wang’s team developed a new tool that combines fluorescent imaging with the gene-editing technology CRISPR to map gene activity within cells. Called FISHnCRISP, the tool revealed the tumor-suppressing gene ZBTB7A is silenced in AML.
“Most drugs right now target the genes that are upregulated in tumor cells, but sometimes it’s very hard to find a therapeutic for that. Instead, we developed this CRISPR-based screen to identify what upregulates tumor-suppressor genes to kill off the tumor,” Wang said.
For a larger version of this image, please click here.
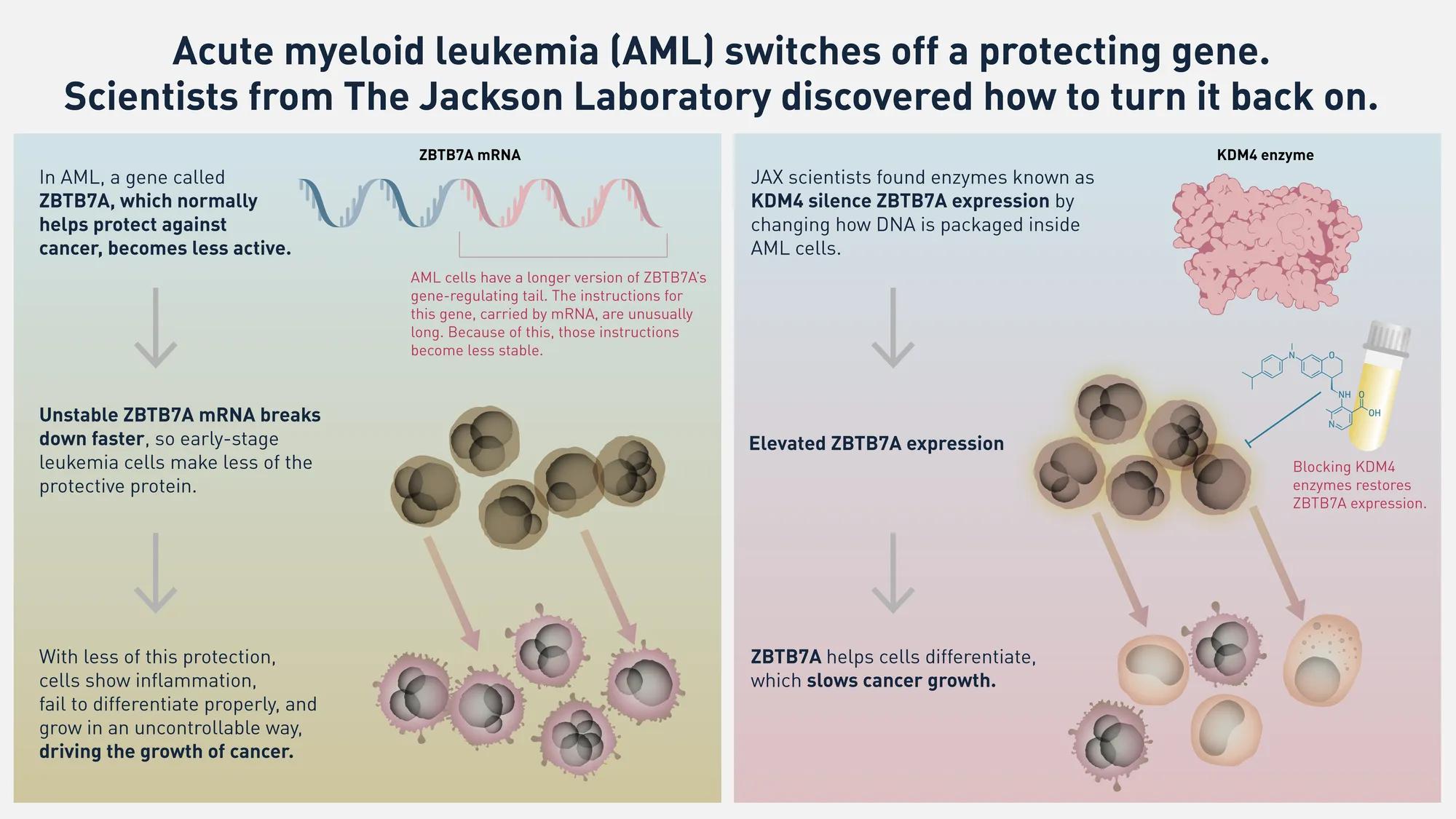
The team discovered AML cells produce a longer version of ZBTB7A’s regulatory tail, a stretch of genetic material that helps control a gene’s activity. The extended tail contains sites that attract a protein called ZFP36L2, which reduces the gene’s activity. Additionally, the team found the group of enzymes known as KDM4 modify how DNA is packaged inside AML cells, effectively silencing ZBTB7A expression.
The study included tests on mice with AML cells taken directly from patients to closely mimic the real disease. When KDM4 enzymes were blocked, ZBTB7A regained its expression, reducing leukemia burden while leaving normal blood formation largely unaffected.
“There are drug candidates out there to inhibit KDM4, and in our study we just repurposed one of them to treat AML cells,” Wang said. “We won’t know unless we test it in clinical trials, but this approach could be better than chemotherapy, because we showed it's not toxic at all to normal blood cells.”
A new differentiation therapy?
More common in older adults, and despite therapeutic advances, AML has a relatively poor prognosis. One of the reasons for this is that AML cells thrive because they remain in an immature state that resembles stem cells, which do not differentiate into other cells. By restoring ZBTB7A expression, the scientists forced the cancer cells into a state in which they grow less aggressively and become more vulnerable.
“We demonstrated that downregulating ZBTB7A causes this hyper inflammatory state that promotes cancer growth,” Wang said. “Now, we’re proposing this epigenetic approach to force AML cells to differentiate into white blood cells that eventually undergo cell death.”
Future studies will focus on refining the approach and determining whether it might be combined with existing treatments. The team is planning to test an experimental drug to target KDM4 currently being tested in a clinical trial for solid tumors.
“We could potentially translate our research into an early phase clinical trial more readily than developing a whole new compound from scratch,” Wang said.
Other authors are Alexander Arnuk, Cuijuan Han, Abimbola E. Lawal, Bofei Wang, Sadik Karma, Zhiping Zhang, Mhd Yousuf Yassouf, Sakthi Harini Rajendran, Harshpreet Chandok, Madeline L. Eller, Sogand Sajedi, Meryl McKenna, Eve Herman, Louisa Hagen, Bettina Nadorp, Zengshuo Mo, Hector Orellana, Aristotelis Tsirigos, Pedro Miura, Hussein A. Abbas, and Iannis Aifantis.
This work was supported by the Jackson Laboratory Cancer Center New Investigator Award (P30CA034196), JAX startup funds, JAX Cancer Center Fast Forward Award, JAX Cancer Center Innovation Pilot Award (P30CA034196), American Society of Hematology (ASH) Scholar Award, Leukemia Research Foundation, and Butler Family Foundation; the JAX Cancer Center Brooks Scholar Award; the American Society of Hematology Scholar Award; the American Heart Association fellowship; the Physician Scientist Award from the MD Anderson Cancer Center and the Cancer Prevention and Research Institute of Texas Individual Investigator Award; the National Institute of General Medical Sciences (grant R35GM138319); the Vogelstein Foundation, the EvansMDS Foundation, MPN Research Foundation, and the National Institutes of Health/National Cancer Institute (2P01CA229086, 5R01CA228135, 5R01CA242020, 1R01hl159175, and 1R01CA271455).
Citation: Arnuk A., Han C., Lawal A.E., et al. Abimbola E., Bofei Wang, Sadik. Epigenetic reactivation of the tumor suppressor ZBTB7A by KDM4 inhibition in human acute myeloid leukemia. Science Translational Medicine (2026). https://www.science.org/doi/10.1126/scitranslmed.ady2936
JAX media contact: Roberto Molar, [email protected], 202-765-5144
About The Jackson Laboratory
The Jackson Laboratory (JAX) is an independent, nonprofit biomedical research institution with a National Cancer Institute-designated Cancer Center. JAX leverages a unique combination of research, education, and resources to achieve its bold mission: to discover precise genomic solutions for disease and empower the global biomedical community in the shared quest to improve human health. Established in Bar Harbor, Maine in 1929, JAX is a global organization with nearly 3,000 employees worldwide and campuses and facilities in Maine, Connecticut, California, Florida, New York, and Japan. For more information, please visit www.jax.org.
Learn more

Study uncovers molecular “switch” behind chemoresistance in blood cancer
JAX scientists are beginning to understand how RNA biology affects resistance to chemotherapy in acute myeloid leukemia.
View more
The Wang Lab at The Jackson Laboratory
The Wang Laboratory at The Jackson Laboratory for Genomic Medicine focuses on understanding gene regulatory mechanisms that influence leukemia survival, differentiation, and therapy response.
View more