Engineering the future of cancer research with patient-derived organ-on-a-chip technology
Article | February 12, 2026

Colorectal cancer is rising among younger adults, often striking people in their 30s and 40s with little warning. While genetics, diet, and lifestyle all play a large role, scientists increasingly suspect that bacteria in the gut could also be a driver of the disease. Daniel Peñarete-Acosta, a postdoctoral associate at The Jackson Laboratory is working on cutting-edge technology to study the interactions between the immune system and the microbiome in colorectal cancer.
Peñarete-Acosta’s work sits at the intersection of engineering, microbiology, and cancer biology. In the Jalili Lab at JAX, he develops organ-on-a-chip platforms using patient-derived tissues to study how bacteria interact with human tumors over long periods of time. The goal is to move beyond correlation and toward causation—understanding not just whether bacteria are associated with cancer, but how they contribute to its development in individual patients.
“To me, the most fascinating thing is the fact that we're developing tools that allow us to study biological interactions in a way that was not possible before at all,” said Peñarete-Acosta.

Traditionally, researchers studying bacteria-cancer interactions relied on simplified cell culture experiments or animal models. Those approaches offered limited windows into complex, long-term interactions. Scientists would expose cancer cells to bacteria to watch the interactions. But after only a few hours, the bacteria would kill the cancer cells. Organ-on-a-chip systems change that dynamic.
Roughly the size of a USB stick, an organ-on-a-chip is a clear plastic device with hollow microchannels that are lined with living human cells. Fluids continuously flow through these channels, creating conditions that mimic blood circulation, breathing motions, or—in the case of Peñarete-Acosta’s work—the physical stresses inside the gut. Unlike static petri dishes, these chips allow scientists to replicate the dynamic environment of the human body where cells are constantly interacting with their neighbor cells, the microbiome, and the body’s immune system.
While bacteria have long been implicated in colorectal cancer, proving their role in humans has been challenging. Using samples taken directly from patients, Peñarete-Acosta can maintain bacterial and tumor interactions for days or even weeks—timescales that more closely resemble what happens in the human body.
“With this technology, we can finally use human samples to collect human-relevant data to prove that there is causation in this relationship between bacteria and cancer, not only correlation,” he said. “With the technology that we have now, we can really start to understand the long-term effects of those interactions.”
The work is technically demanding, requiring extensive iteration and engineering. Peñarete-Acosta has personally designed and built multiple generations of these platforms, scaling them from early prototypes to systems capable of running many experiments simultaneously. His current rig has 16 experiments running at once.
The path to personalized medicine
Peñarete-Acosta’s path to cancer research wasn’t a straight line. He began his undergraduate training in chemical engineering, doubling with microbiology and initially focusing on biotechnology and biofuels. A senior design project at Texas A&M University introduced him to bacterial pathogenesis and microfluidic technology—the ability to precisely control fluids at microscopic scales. That experience would later prove foundational. But it was a personal loss during his graduate training that ultimately redirected his scientific focus.
But after his grandmother unexpectedly passed away from cancer, he shifted his Ph.D. focus and never looked back. “I just knew my real passion was to do biomedical research,” he said.
With the support of his advisor, Peñarete-Acosta transitioned into a biomedical engineering Ph.D. program, where he spent six years combining microfluidics, computational simulations, and fluid dynamics to study cancer-related biological processes. That winding path eventually brought him to the Jalili Lab at JAX in 2023.
He was recently awarded the Robert E. Leet and Clara Guthrie Patterson Trust Mentored Research Award, which will provide $200,000 over the next two years to support his work.
A major advantage of working at JAX, Peñarete-Acosta said, is access to human patient samples from our partners at UConn Health. His current work use tissue collected during colorectal cancer surgeries, including both tumor samples and normal adjacent tissue from the same individual.
“That really allows us to study the diversity of the disease but also a more personalized focus,” he said. It helps researchers understand why one person gets cancer over another—and what the best treatment for each person could be.
Peñarete-Acosta said he believes in the next 10 years, we’ll see more and more researchers will rely on organ-on-a-chip technology with patient-derived samples to help accelerate the discovery process. Understanding the mechanisms that cause disease can help scientists in prevention and intervention.
Learn more
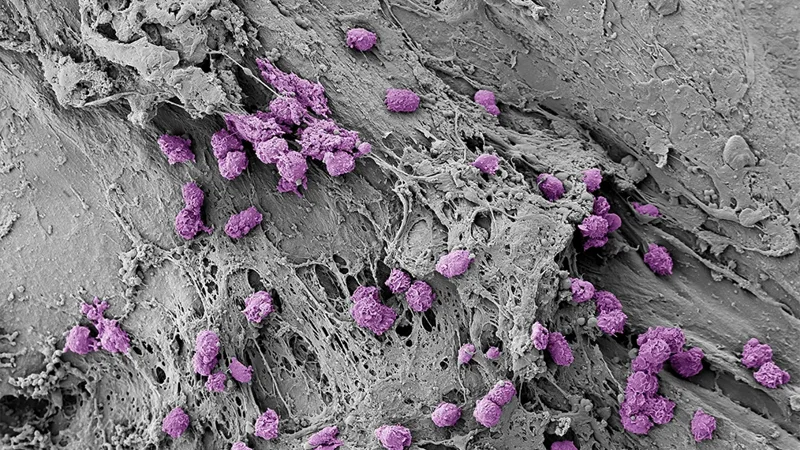
The Jalili Lab at The Jackson Laboratory
The Jalili Research Group at The Jackson Laboratory (JAX) is focused on interrogating the host immunity, microbiome and their interface using different engineering tools in the context of infectious diseases, autoimmunity and cancer.
View more
Day in the Life of JAX Postdoc Daniel Peñarete, Ph.D.
What’s it like to be a JAX trainee? Follow along for a day to see life as a postdoctoral associate in the Jalili Lab at JAX.
