Using mathematical modeling to target infections
Article | September 4, 2018
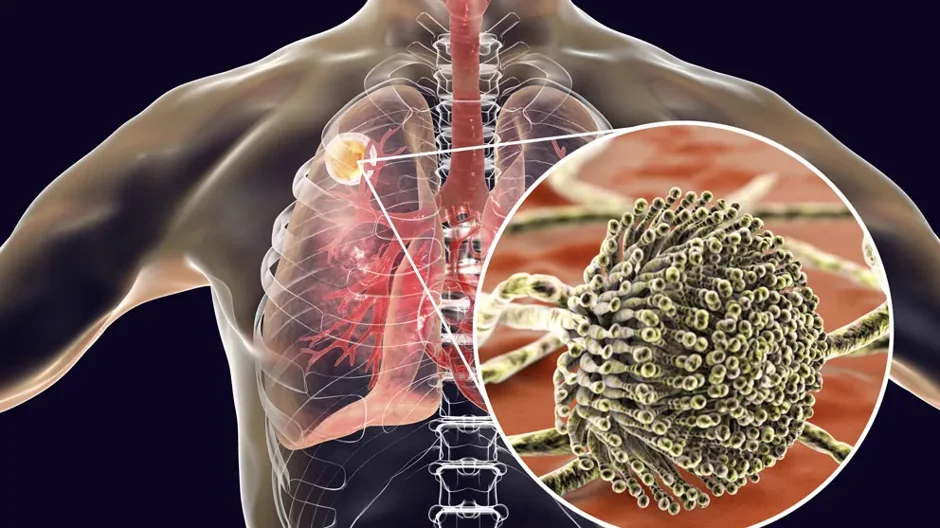
No one is ever pleasantly surprised to find mold growing on food that has been left in the fridge too long. But everyday there is plenty of mold around us that we don’t see, including hundreds of spores of some types of invisible mold that we unknowingly inhale.
While this probably sounds pretty alarming and disgusting, Aspergillus fumigatus is not harmful to most people. However, for someone with a weakened immune system, this fungus poses serious health dangers.
Mathematical modeling is a powerful technology that can help us understand and control complex regulatory mechanisms.
Reinhard Laubenbacher, Ph.D., joint faculty member at UConn Health and The Jackson Laboratory for Genomic Medicine, has received more than $3 million from the National Institutes of Health National Institute of Allergy and Infectious Diseases to use mathematical and computational tools to explore new potential therapeutic targets to treat those affected by invasive aspergillosis.
When the otherwise harmless fungus invades the lungs of people with compromised immune systems, it can cause severe respiratory problems. Serious diseases that frequently occur as comorbidities with invasive aspergillosis in immunocompromised patients are tuberculosis and chronic obstructive pulmonary disease.
To make matters worse, since immunocompromised patients are unable to clear the spores from their system in the way most of us can, the fungus can seep into the bloodstream and affect other internal organs like the heart, brain, and kidneys.
An additional concern is that patients who require organ or bone marrow transplants receive immunosuppressive therapies in order to increase the body’s ability to accept a transplanted organ. This has led to an increase in fatalAspergillus infection.
Similarly, chemotherapy cancer treatment weakens the patient’s immune system temporarily as cancerous cells and other healthy, rapidly dividing cells like those in bone marrow, which produce antibody-fighting white blood cells, are damaged.
While most current therapies focus on understanding the nature of the pathogenic fungus, Laubenbacher is interested in considering the components of the host’s defense system.
Our bodies need iron to facilitate the transportation of oxygen from our lungs by our red blood cells, and many other processes. Likewise, pathogens need iron for growth and virulence. Restricting the availability of iron to pathogens likeAspergillus fumigatus is one of the key early mechanisms the immune system uses to fight microbial invaders.
Unfortunately, most pathogens, such as Aspergillus fumigatus, have been evolving to find ways to scavenge iron from the host, circumventing this defense. A compromised immune system gives the fungus even more of an advantage in this “battle over iron.”
The model Laubenbacher will develop focuses on simulating the role of iron inAspergillus fumigatus infection by modeling a variety of mechanisms at multiple scales that contribute to this process.
“Mathematical modeling is a powerful technology that can help us understand and control complex regulatory mechanisms,” Laubenbacher says. “While it is commonly used in industry and business, applications in biomedicine are relatively recent. We hope to bring this capability to the improved control of devastating fungal infections.”
This work could aid the development of new treatments for this infection that may be able to improve host iron sequestration mechanisms.
Laubenbacher is partnering with the pulmonary immunology laboratory of Borna Mehrad at the University of Florida for this work.
Laubenbacher received his Ph.D. in mathematics from Northwestern University in 1985. His current research interests include the development of mathematical algorithms and their application to problems in systems biology, in particular the development of multi-scale models of disease processes. Current applications include infectious diseases and cancer.
This project is NIH Grant No.: 1 R01 AI135128-01
